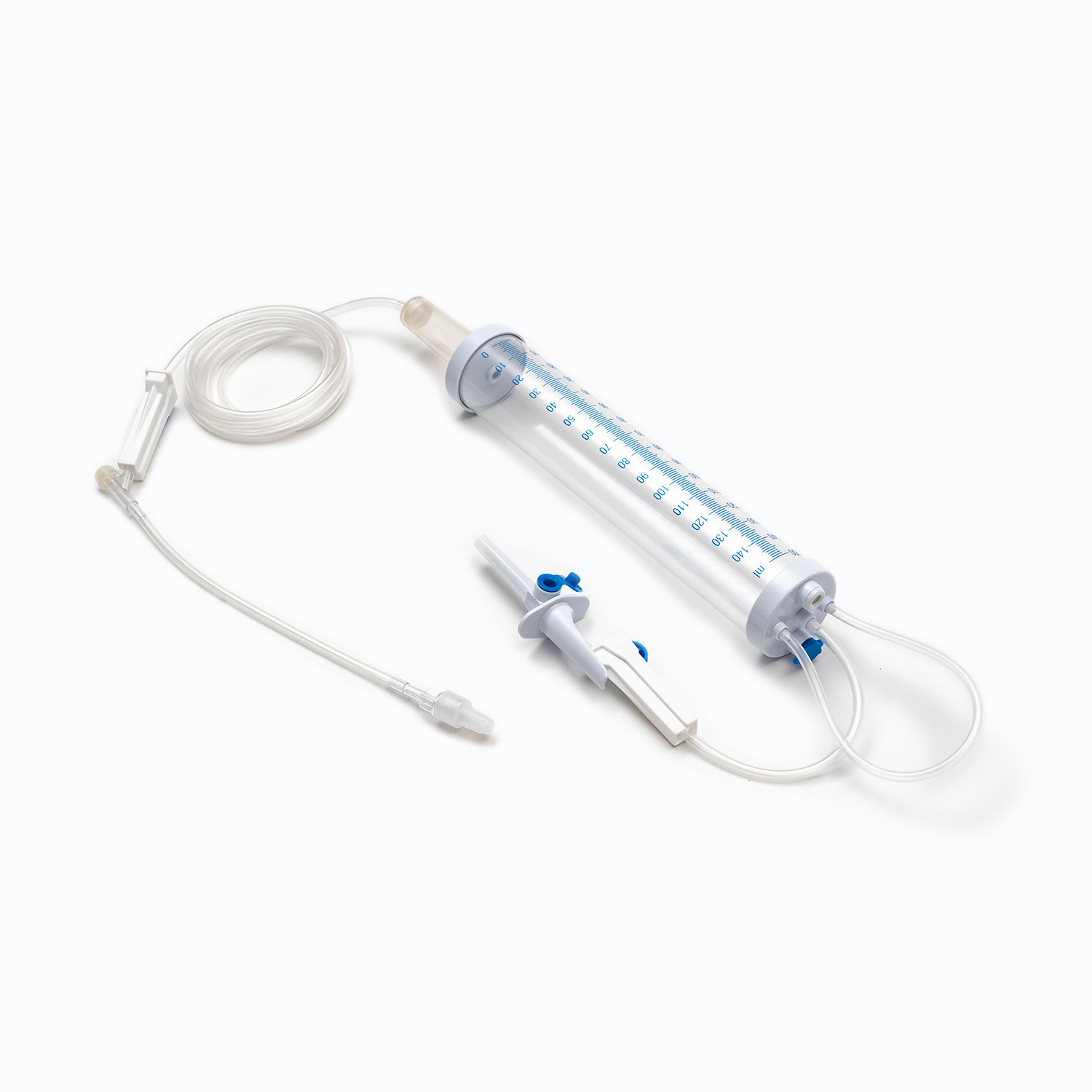
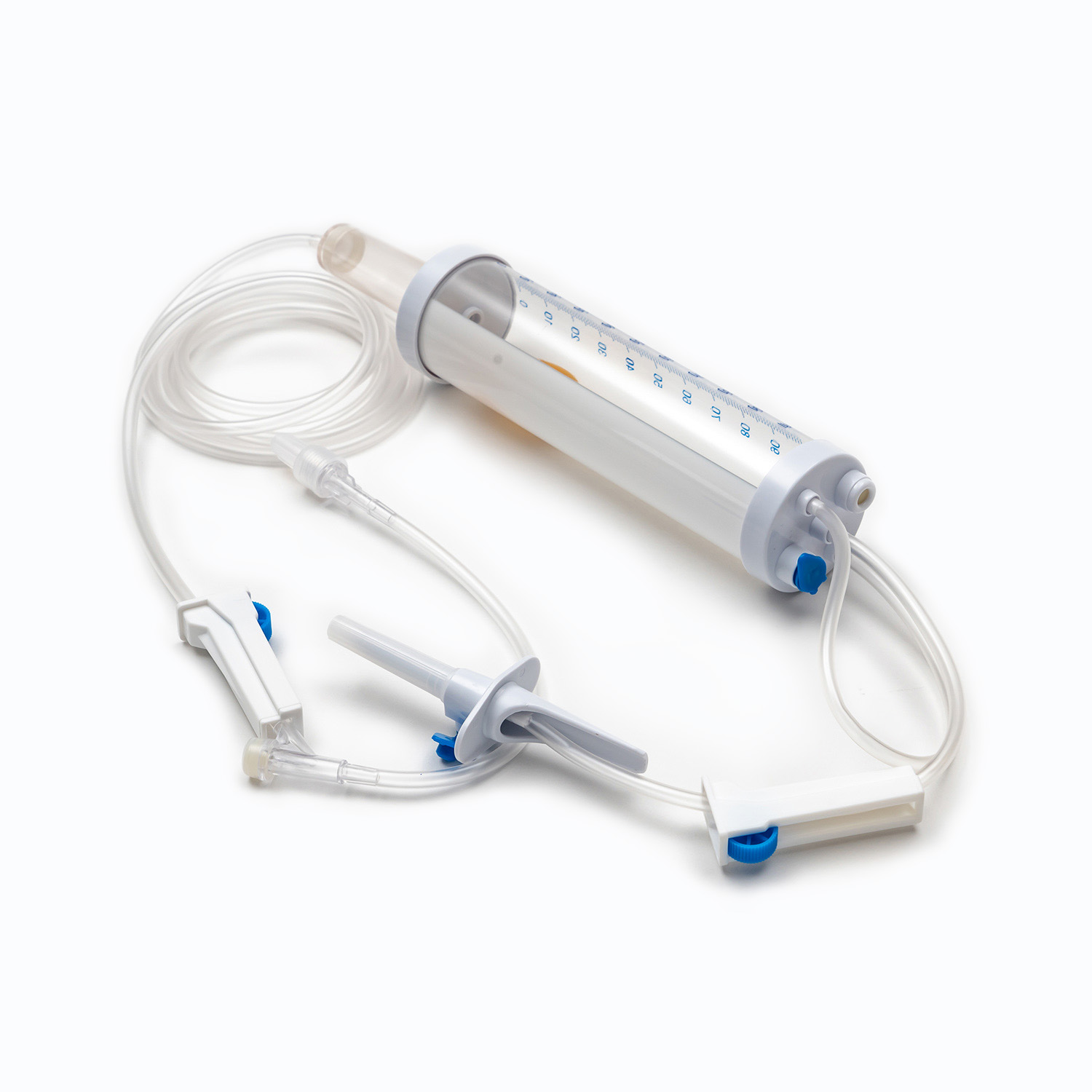
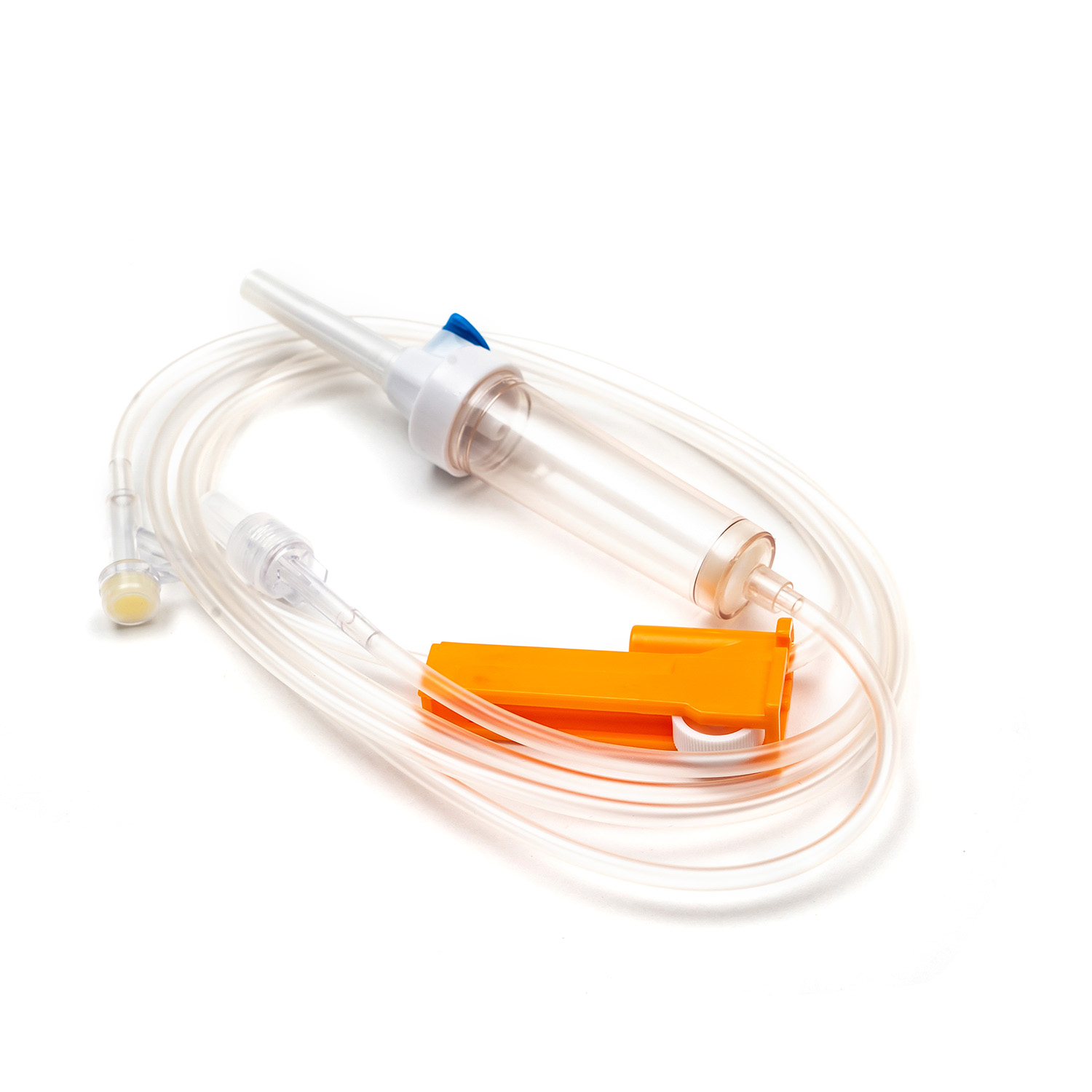
How Can You Prevent Infections When Using a Urinary Catheter?
May 08,2026
Urinary Catheter Use is a Safe and Effective Medical Intervention When Properly Managed
The direct and definitive conclusion regarding the use of a urinary catheter is that it is a highly safe, effective, and often indispensable medical tool when appropriate clinical indications are present, and strict hygiene protocols are followed. While the insertion of a foreign body into the urinary tract inherently carries a risk of infection, modern medical guidelines, evidence-based nursing practices, and advanced catheter materials have significantly minimized these dangers. The development of urinary tract infections is largely preventable through aseptic insertion techniques, proper securement, and timely removal. For patients experiencing acute urinary retention, requiring precise surgical fluid monitoring, or managing severe incontinence, the benefits of a urinary catheter far outweigh the potential risks. Understanding the specific type of catheter required, mastering the daily care routine, and recognizing the early signs of complications empower both healthcare providers and patients to utilize this device safely and effectively without unnecessary anxiety.
Understanding the Primary Clinical Indications for Catheterization
The decision to insert a urinary catheter is never taken lightly in clinical practice. It is a targeted intervention designed to address specific physiological failures or monitoring needs. The most prominent indication is acute urinary retention, a painful condition where the bladder fills with urine but the patient is entirely unable to void. This can occur due to an enlarged prostate blocking the urethra, severe constipation, or neurological conditions that disrupt the nerve signals between the brain and the bladder. In these scenarios, a urinary catheter acts as an immediate relief valve, preventing the backflow of urine into the kidneys which can cause permanent renal damage.
Beyond acute retention, catheters are frequently utilized in surgical and critical care environments. During major operations or in intensive care units, accurate measurement of urine output is vital. Urine production is a direct indicator of kidney perfusion and overall circulatory volume. By utilizing a urinary catheter, medical staff can monitor exactly how much urine is produced every hour, allowing for rapid adjustments to intravenous fluid therapy or medication dosages. Furthermore, for patients with severe mobility issues, end-stage neurological diseases, or profound cognitive impairments who cannot control their bladder function, a catheter provides a long-term management strategy that protects the skin from constant exposure to moisture and prevents the development of severe pressure ulcers.
Categorizing the Main Types of Urinary Catheters
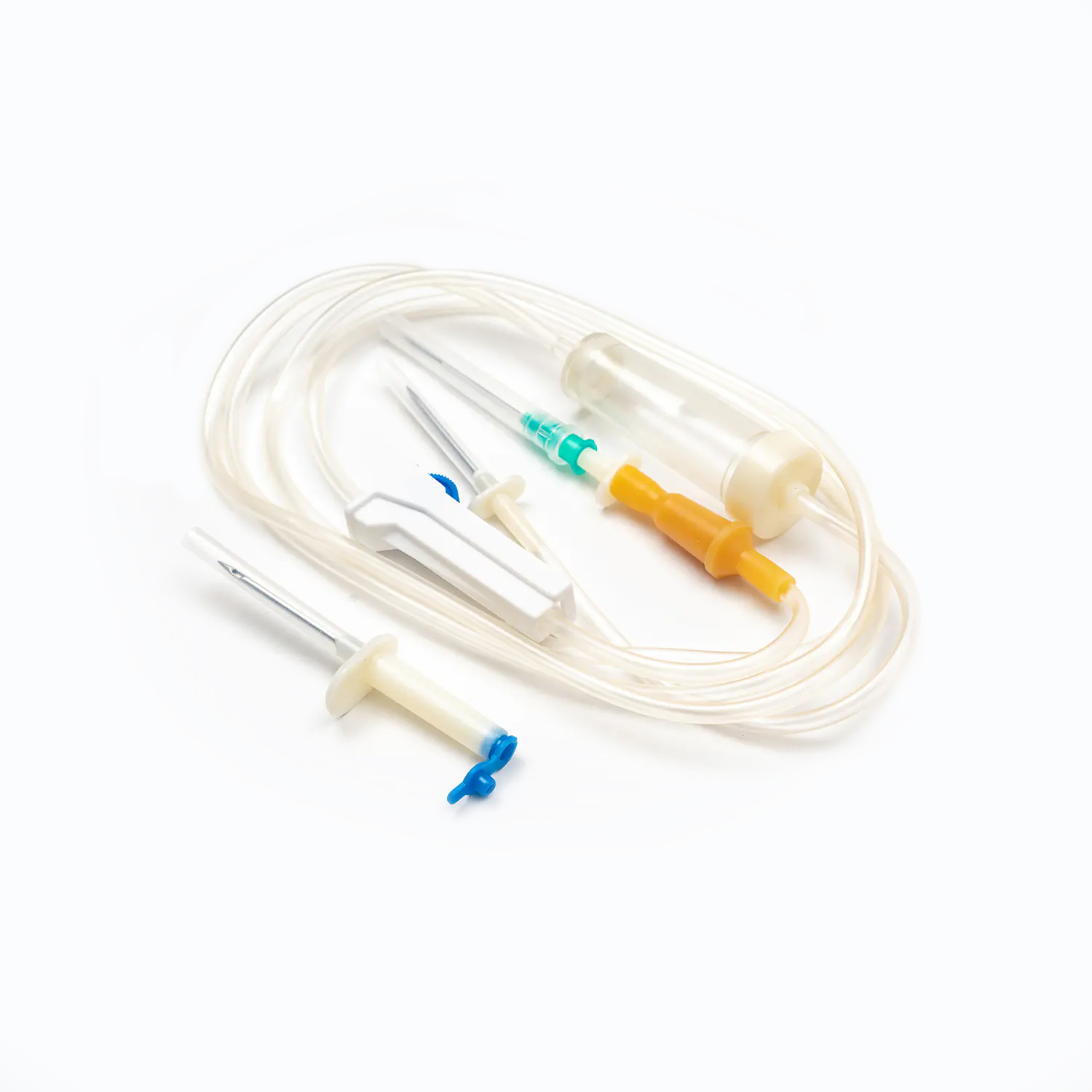
Not all urinary catheters are created equal. They are broadly categorized by the duration of intended use and the specific anatomical pathway they utilize. Selecting the wrong type can lead to unnecessary discomfort, tissue damage, or a spike in infection rates. Healthcare providers must carefully assess the patient's medical status, anticipated length of need, and anatomical considerations before making a selection.
Short-Term Versus Long-Term Catheters
The distinction between short-term and long-term devices is primarily based on the material composition. Short-term catheters are typically made from polyvinyl chloride (PVC) or basic latex. These materials are stiff, which makes them easier to insert, but they begin to degrade and become brittle if left in the bladder for more than a few weeks. The degradation process releases particles that can irritate the bladder lining and encourage bacterial colonization. Long-term catheters, on the other hand, are manufactured from silicone or specially coated latex. Silicone is entirely biocompatible, meaning it does not provoke a significant immune or inflammatory response, and it remains flexible and structurally sound for several weeks to months, making it the standard choice for chronic indwelling use.
Indwelling, Intermittent, and External Pathways
The functional design of the catheter dictates how it interacts with the body. An indwelling catheter, often referred to as a Foley catheter, is the most recognizable type. It is inserted through the urethra into the bladder and features a small balloon at the tip that is inflated with sterile water once inside. This balloon anchors the catheter in place, allowing it to remain securely positioned for continuous drainage into a collection bag. Intermittent catheters are fundamentally different; they have no balloon and are not designed to stay in the body. A healthcare professional or the patient inserts the catheter multiple times a day to drain the bladder and then immediately removes it. This method closely mimics natural bladder function and is widely considered the gold standard for managing chronic urinary retention in patients who have the physical dexterity to perform the task. Finally, external catheters are male-specific devices that resemble a condom and roll over the penis, connecting to a drainage bag. They are entirely non-invasive and are primarily used for men with incontinence who do not have urinary retention.
| Catheter Type | Primary Use Case | Duration of Use |
|---|---|---|
| Foley (Indwelling) | Surgery, acute retention, critical care | Short to Long-term |
| Intermittent | Chronic retention, spinal cord injuries | Single use, multiple times daily |
| External (Condom) | Male incontinence without retention | Changed daily |
Essential Protocols for Daily Care and Maintenance
The presence of an indwelling urinary catheter requires rigorous daily maintenance to ensure patency and prevent complications. The urinary tract is normally a sterile environment, but the presence of a catheter provides a direct highway for bacteria to enter the bladder. Therefore, the foundational principle of catheter care is maintaining a closed drainage system. This means that the connection between the catheter tube and the drainage bag should never be disconnected unless necessary for changing the bag. Breaking this seal introduces air and environmental pathogens directly into the urinary tract.
Hygiene practices surrounding the catheter must be meticulous but gentle. The area where the catheter exits the body—typically the urethral meatus—should be cleaned gently with warm water and a mild soap during daily bathing. Harsh antiseptic solutions, such as concentrated iodine or alcohol, should be avoided as they can irritate the delicate mucous membranes, cause microscopic tears, and actually make the tissue more susceptible to bacterial invasion. The drainage bag poses its own set of rules. It must always be positioned below the level of the bladder, whether the patient is lying in bed, sitting in a chair, or walking. Gravity is the mechanism that allows urine to flow out of the bladder; if the bag is raised above the bladder, urine can flow backward, a phenomenon known as reflux, which can carry bacteria from the contaminated bag directly back into the kidneys. The bag should also be emptied regularly when it is about half to two-thirds full to prevent excessive weight from pulling on the catheter and causing urethral trauma.
Strategies to Prevent Catheter-Associated Urinary Tract Infections
Catheter-associated urinary tract infections (CAUTIs) are among the most common hospital-acquired infections globally. However, the vast majority of these infections are entirely preventable through a layered approach of vigilance and protocol adherence. The first line of defense is strict adherence to aseptic technique during the initial insertion. This involves the use of sterile gloves, sterile drapes, and a sterile no-touch technique where the clinician handles only the sterile catheter and avoids any contact with non-sterile surfaces or the patient's skin after crossing the urethral opening.
Perhaps the most impactful prevention strategy is the practice of daily necessity review. Every single day a patient has a urinary catheter, the medical team should evaluate whether it is still strictly required. Studies consistently show that the risk of developing a CAUTI increases exponentially with each additional day the catheter remains in place. By removing the device as soon as the patient can void naturally or when accurate hourly monitoring is no longer needed, the overall infection rate drops dramatically. Additionally, securing the catheter properly to the patient's thigh or abdomen is a critical, often overlooked intervention. A secure catheter prevents excessive movement and tugging at the urethral opening. This micro-motion causes friction and inflammation, creating microscopic abrasions where bacteria can easily attach and multiply. Utilizing a specialized securement device rather than standard adhesive tape provides stable anchoring while allowing for easy adjustment and skin inspection.
Recognizing and Managing Potential Complications
Even with excellent care, complications can arise, and early recognition is key to preventing severe outcomes. The most frequently encountered issue, aside from infection, is catheter blockage. Over time, minerals in the urine, particularly calcium and magnesium, can precipitate and form crystals on the surface of the catheter. This encrustation gradually narrows the lumen of the tube, eventually stopping urine flow entirely. A blocked catheter can cause acute pain, bladder spasms, and a dangerous buildup of pressure. If flushing the catheter with sterile saline does not resolve the blockage, the catheter must be replaced immediately by a trained professional. Patients or caregivers should never attempt to forcefully irrigate a blocked catheter, as this can rupture the bladder or push infected debris back into the kidneys.
Other complications include trauma and leakage. Trauma can occur if the catheter is pulled violently, potentially tearing the urethra or causing the retention balloon to become lodged in the urethra. If resistance is felt during insertion or removal, the procedure must be stopped immediately to avoid catastrophic damage. Urine leakage around the outside of the catheter is another common issue. While it can simply indicate that the catheter is too small or that bladder spasms are occurring, it can also be a warning sign of a blocked tube or a severe infection causing intense bladder inflammation. Any sudden onset of fever, severe lower abdominal pain, cloudy or foul-smelling urine, or significant bleeding around the catheter site requires immediate medical evaluation.
Critical Considerations for Patient Lifestyle and Comfort
Living with a urinary catheter, whether for a few days or several months, requires significant psychological and lifestyle adjustments. One of the primary concerns for patients is how the device will affect their mobility and daily activities. The good news is that with the right equipment, patients with indwelling catheters can remain highly active. Leg bags are designed specifically for daytime use; they strap securely to the thigh under clothing, are discreet, and hold a sufficient volume of urine to allow for trips outside the home, exercise, and social activities. At night, the leg bag is typically swapped for a larger capacity night bag that hangs on the frame of the bed, ensuring uninterrupted sleep without the need to wake up to empty a small bag.
Fluid intake is another vital lifestyle consideration. There is a common misconception that patients with catheters should drink less fluid to reduce the frequency of bag emptying. In reality, the opposite is true. Adequate daily hydration is essential to flush bacteria out of the bladder and prevent the formation of mineral crystals that cause blockages. Patients should aim for a normal, healthy intake of water unless specifically restricted by a doctor for other conditions, such as heart failure or severe kidney disease. Furthermore, sexual activity requires careful consideration and communication. While it is entirely possible to maintain intimacy with a catheter in place, it requires patience, positioning adjustments, and ensuring the catheter is securely taped out of the way to prevent painful pulling. Open discussions with healthcare providers about these intimate concerns are crucial for maintaining overall quality of life and mental well-being during catheter therapy.
The Process of Safe Removal and Post-Removal Monitoring
The removal of a urinary catheter is just as clinically significant as its insertion. The process is generally quick and involves a syringe inserted into the balloon inflation port to withdraw the sterile water, causing the anchoring balloon to deflate and collapse. Once deflated, the catheter is smoothly and gently pulled out. Patients may feel a brief sensation of pressure or slight discomfort as the tube passes through the urethra, but it should not be intensely painful. Following removal, the body needs time to re-establish its natural urinary rhythms.
Post-removal monitoring is a critical phase where complications can still arise. The most common issue is urinary retention after removal, meaning the bladder has become so accustomed to the catheter continuously draining it that the detrusor muscle has temporarily lost its ability to contract forcefully enough to expel urine. If a patient has not voided within six to eight hours of catheter removal, or if they experience extreme discomfort and a visibly distended bladder, medical intervention is required, as the catheter may need to be reinserted temporarily. Another expected phenomenon is post-void residual dribbling, where the patient urinates normally, but a small amount of urine leaks out afterward. This is caused by the urethra being slightly stretched and weakened by the prolonged presence of the catheter. This dribbling usually resolves spontaneously within a few days as the urethral muscles regain their tone. Patients are also encouraged to practice pelvic floor exercises during the recovery phase to accelerate the restoration of urinary control and continence.
Special Considerations for Intermittent Self-Catheterization
For patients managing chronic conditions like spinal cord injuries, multiple sclerosis, or spina bifida, intermittent self-catheterization (ISC) is often the preferred long-term strategy. Unlike indwelling catheters, ISC allows the patient to maintain a completely natural lifestyle between catheterizations, preserving bladder capacity and significantly reducing the risk of bacterial colonization. The core philosophy of ISC is that the patient acts as their own nurse, taking responsibility for their bladder health. To succeed, patients must be thoroughly educated on hand hygiene, the anatomy of their own body, and the physical mechanics of the procedure.
The technique requires the use of clean, non-sterile catheters, as opposed to the sterile environment required for initial indwelling insertion. The patient washes their hands thoroughly with soap and water, cleanses the genital area, and gently advances the lubricated catheter until urine flows. Once the flow stops, the catheter is slowly withdrawn to ensure the bladder is empty. A critical component of ISC success is adherence to a strict schedule. Patients are typically instructed to catheterize every four to six hours, adjusting based on fluid intake, to ensure the bladder never overfills. Consistent timing prevents bladder overdistension, which can lead to kidney damage and eliminates the risk of stretch-related muscle atrophy. By mastering this technique, patients regain profound independence, freeing themselves from the constant presence of drainage bags and the restrictive lifestyle associated with indwelling urinary catheters.
Advancements in Catheter Technology and Materials
The evolution of urinary catheter technology has consistently focused on reducing the biological burden placed on the patient's body. Traditional latex catheters, while flexible, pose a significant risk of allergic reactions and are highly susceptible to bacterial adherence. The shift toward silicone as a primary material has drastically improved biocompatibility. Silicone does not contain allergenic proteins, and its ultra-smooth surface makes it remarkably difficult for bacteria to anchor themselves and form biofilms—a protective matrix that bacteria build to shield themselves from antibiotics and the immune system.
Beyond material changes, surface coatings represent the cutting edge of catheter innovation. Modern specialized catheters are frequently coated with antimicrobial agents, such as silver alloy or nitrofurazone, which are slowly released into the surrounding tissues to create a hostile environment for bacteria. Hydrogel coatings are another significant advancement; these coatings absorb water and create a slick, highly lubricated surface that drastically reduces the friction between the catheter and the urethral wall during both insertion and while the catheter remains in the body. This reduction in friction directly correlates with decreased tissue trauma, less inflammation, and a subsequent drop in infection rates. Furthermore, the engineering of the catheter tips has seen refinement. The introduction of coude tip catheters, which feature a slightly curved tip, allows for easier navigation around anatomical obstacles like an enlarged prostate, reducing the need for forceful insertion and minimizing the risk of creating false passages or causing severe bleeding. These technological strides continue to elevate the safety profile of urinary catheterization.
Debunking Common Misconceptions Surrounding Catheter Use
The subject of urinary catheters is clouded by numerous myths that can cause unnecessary distress for patients and lead to poor decision-making. One of the most pervasive myths is that having a catheter means the patient is permanently incontinent or that their bladder will permanently stop working. In reality, the bladder is a highly resilient muscle. Even after months of indwelling catheterization, the bladder usually retains the ability to regain its function once the catheter is removed and the patient undergoes rehabilitative voiding. Another dangerous misconception is that if a patient feels the urge to urinate while catheterized, something is wrong. Patients must understand that the urethral balloon sits at the bladder neck, and the presence of the catheter continuously triggers the stretch receptors in the bladder wall, sending signals to the brain that mimic the normal sensation of a full bladder. This is a normal anatomical response, not a sign of a blockage or malfunction.
A third common fallacy involves the cleaning of the drainage bags. Many caregivers believe that adding harsh disinfectants, bleach, or vinegar solutions into the drainage bag will keep it sterile and prevent infections. This practice is strongly discouraged in modern medical guidelines. Adding these chemicals can cause a chemical reaction with the urine, creating toxic gases or crystalline precipitates that can actually block the catheter. The most effective and safest way to manage bag cleanliness is to simply rinse it with warm water and allow it to air dry completely. Disposable bags should be discarded according to the manufacturer's schedule, usually every few days to a week, depending on the type. By dispelling these myths through comprehensive patient education, healthcare providers can significantly improve the patient experience, reduce anxiety, and foster a collaborative environment where catheters are managed safely and effectively based on evidence rather than folklore.



 English
English Français
Français русский
русский Español
Español