How Do Safety Dental Needles Protect Both Patients and Dentists?
Apr 15,2026
Dental Needles Are Indispensable for Painless and Effective Local Anesthesia in Dentistry
In the realm of modern dental care, the dental needle stands as a fundamentally critical instrument that directly determines the patient's experience and the clinician's ability to perform complex procedures. Without the precise and reliable delivery of local anesthetics made possible by these specialized needles, essential treatments ranging from routine cavity fillings to advanced surgical extractions would be associated with excruciating pain. The primary conclusion is that a high-quality dental needle is the definitive bridge between advanced anesthetic solutions and effective pain management, making it absolutely indispensable for any successful dental procedure. By creating a clear, unimpeded pathway through soft tissues, the dental needle ensures that the anesthetic agent is deposited in the exact anatomical location required to block nerve transmission, thereby rendering the patient comfortable and cooperative throughout the treatment process.
The evolution of this tool has transformed dentistry from a historically feared profession into a highly refined medical discipline focused on patient comfort. Understanding the intricate design, appropriate selection, and strict safety protocols associated with dental needles allows both practitioners and patients to appreciate the rigorous standards maintained in contemporary clinical environments. This comprehensive exploration will delve into the structural components, the various gauges available for different clinical scenarios, the techniques that minimize discomfort, and the critical environmental and safety considerations surrounding their use and disposal.
Anatomical Structure and Engineering of a Dental Needle
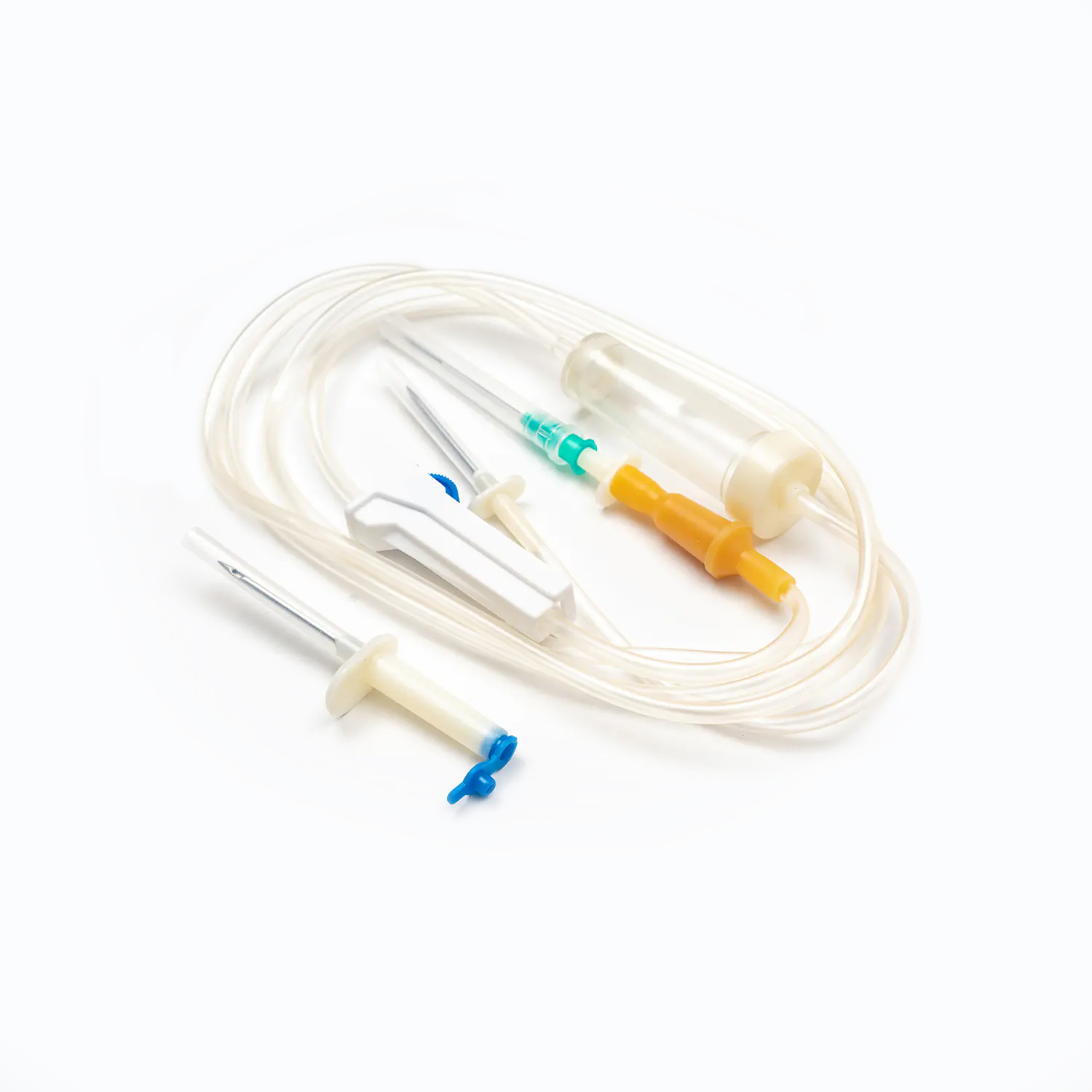
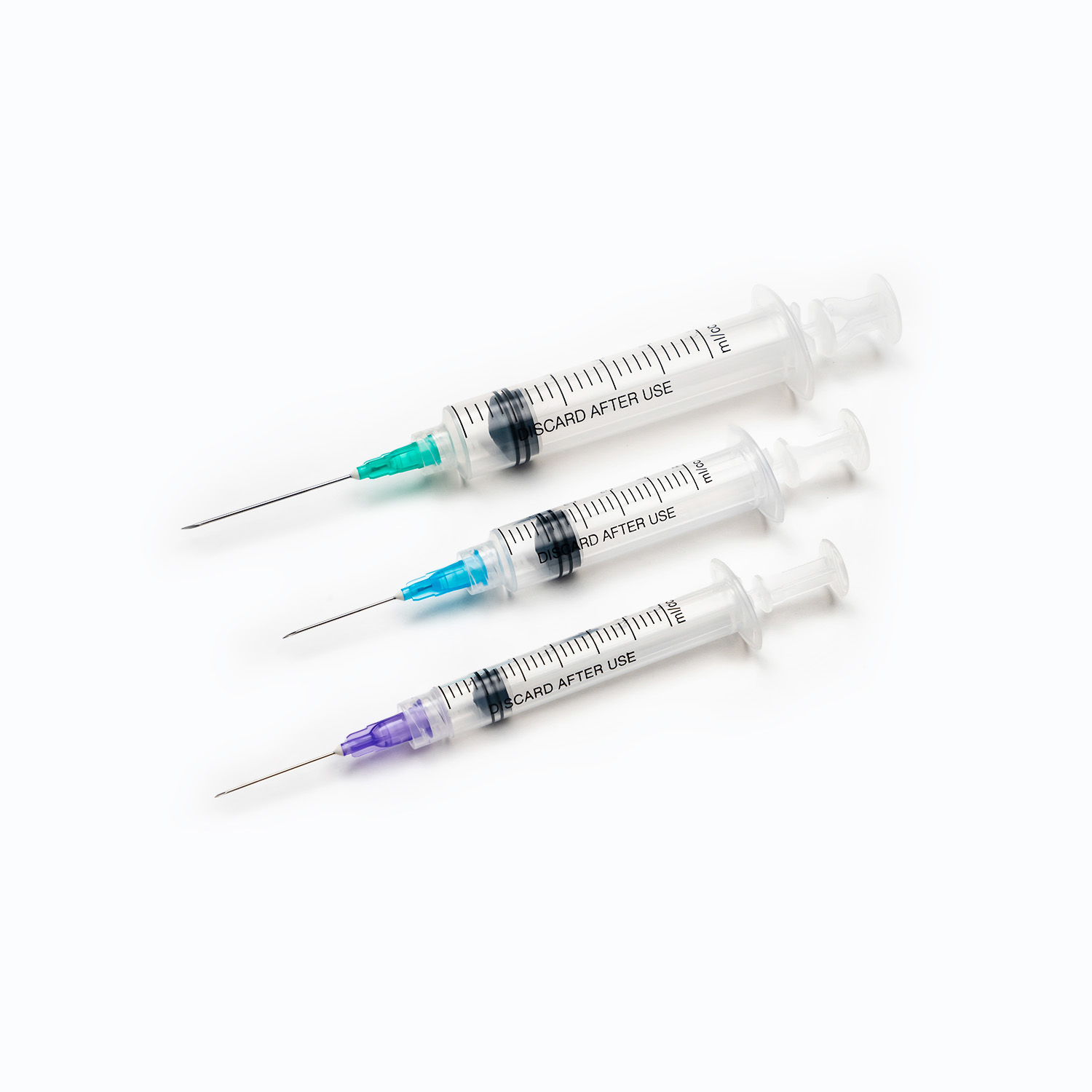
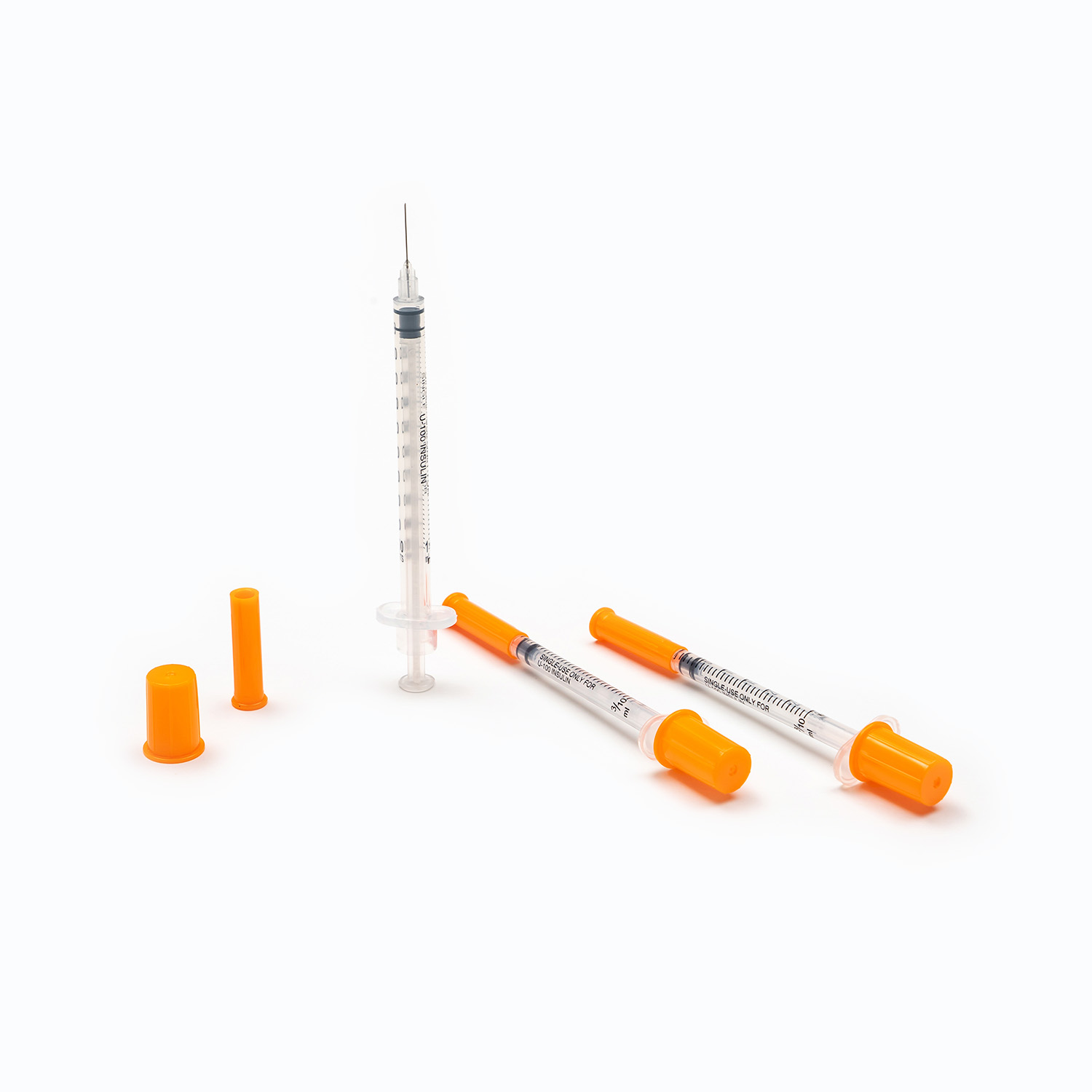
A dental needle is far more than a simple hollow tube; it is a carefully engineered medical device composed of several distinct parts, each serving a specific mechanical purpose. The main components include the hub, the shank, the needle shaft, and the bevel. The hub is typically made of medical-grade plastic or metal and serves as the locking mechanism that attaches the needle securely to the dental syringe. A friction-fit or threaded design ensures that the needle does not detach under the high pressures generated during injection.
The shaft is the long, hollow cylindrical portion of the needle, usually crafted from stainless steel to provide a balance of flexibility and strength. This flexibility is crucial because it allows the needle to navigate through the elastic tissues of the oral cavity without breaking if the patient moves slightly. At the tip of the shaft lies the bevel, which is the slanted, sharpened end of the needle. The geometry of the bevel is specifically designed to part tissue fibers cleanly rather than tearing them, which is the primary mechanical factor in reducing injection pain. A precisely honed bevel creates a narrow, linear incision in the mucosa, significantly lowering the resistance and subsequent discomfort experienced by the patient.
The Significance of the Bevel Design
The bevel of a dental needle is categorized by its length and angle, which dictates how the needle penetrates the tissue. A long bevel features a more gradual slant, resulting in a narrower puncture wound and a more comfortable insertion. Conversely, a short bevel has a steeper angle, which may be preferred in specific techniques where a more abrupt tissue penetration is necessary to reach the target area without the needle bending. The choice of bevel design directly influences the tactile feedback the dentist receives, allowing them to feel the distinct layers of tissue being traversed, such as the mucosa, submucosa, and muscle, ensuring accurate placement of the anesthetic solution.
Understanding Needle Gauges and Their Clinical Applications
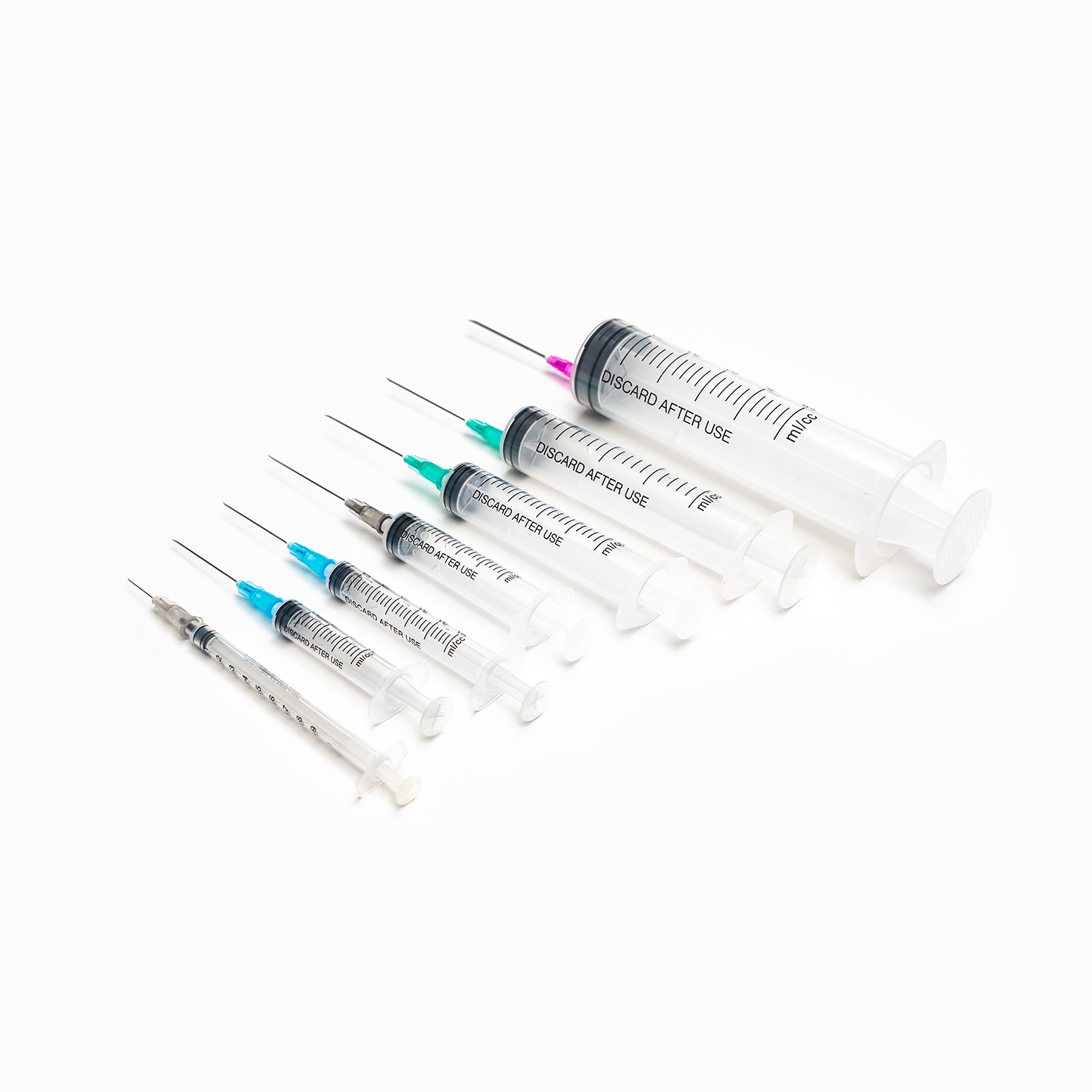
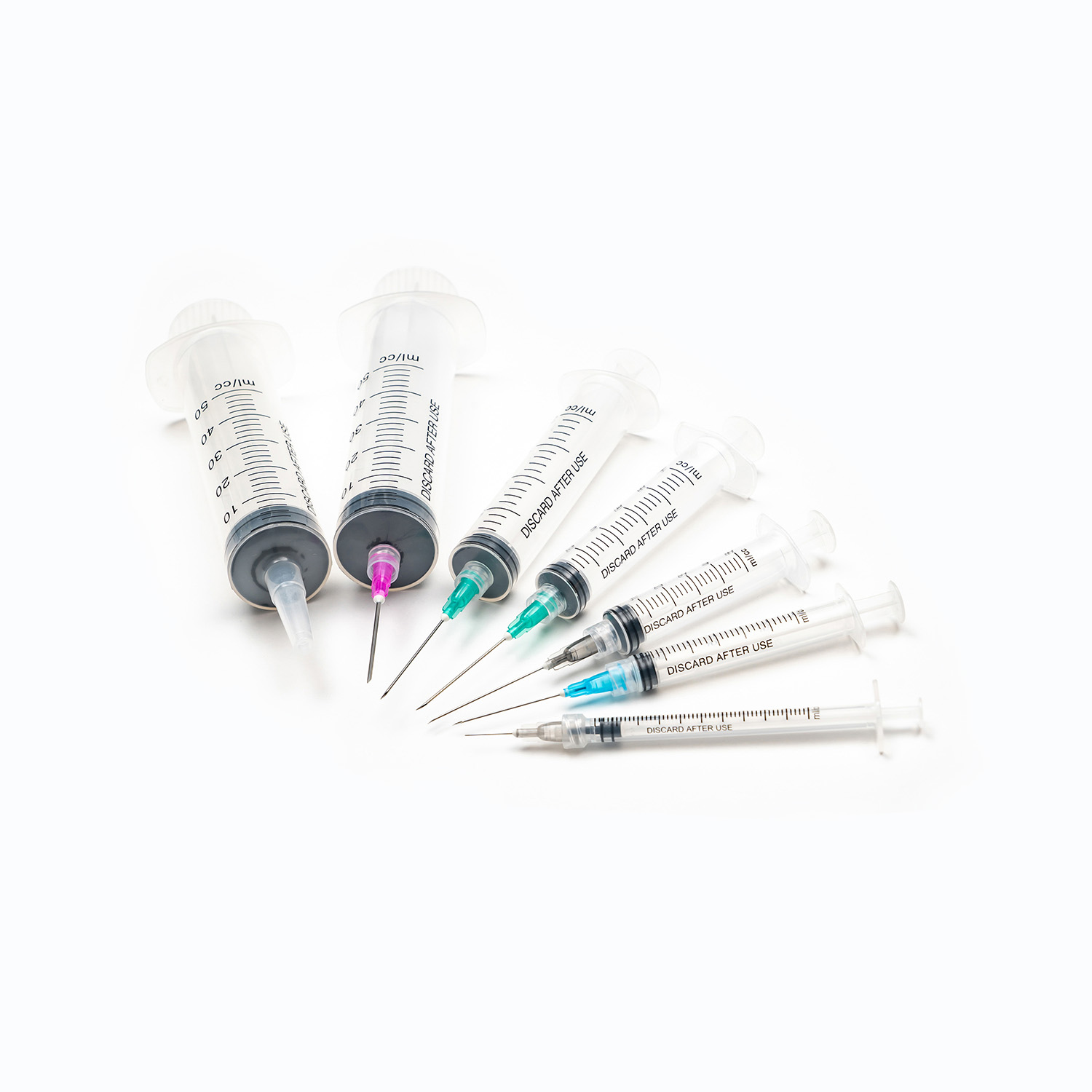
The term "gauge" refers to the outer diameter of the dental needle, and it is a critical factor in determining the flow rate of the anesthetic and the level of discomfort the patient will feel. The gauge system is counterintuitive: a higher gauge number indicates a thinner needle, while a lower gauge number indicates a thicker needle. In modern dentistry, the most commonly utilized sizes are 25-gauge, 27-gauge, and 30-gauge. The selection of the appropriate gauge is a clinical decision based on the specific type of injection required, the viscosity of the anesthetic solution, and the density of the tissues being penetrated.
| Needle Gauge | Relative Diameter | Primary Clinical Use | Flow Characteristics |
|---|---|---|---|
| 25-Gauge | Larger | Deep block injections, dense tissue | Faster, smoother flow |
| 27-Gauge | Moderate | Standard block and infiltration | Balanced flow and control |
| 30-Gauge | Smaller | Superficial infiltration, sensitive areas | Slower, requires more pressure |
Thinner needles, such as the 30-gauge, are generally perceived as less painful by patients because they create a smaller puncture wound in the mucosa. However, their reduced diameter significantly increases the resistance to flow. When a dentist uses a 30-gauge needle, they must apply greater pressure on the syringe plunger to express the anesthetic. This increased pressure can sometimes lead to a less controlled injection, potentially causing tissue trauma if the solution is delivered too rapidly. Therefore, while thinner needles offer comfort during the initial puncture, they require highly developed technique and are not universally suitable for all injection types.
Conversely, a 25-gauge needle provides excellent, unrestricted flow, making it ideal for block anesthesia—such as an inferior alveolar nerve block—where the anesthetic must be deposited deep into tissue spaces near large nerve bundles. The slightly larger diameter is well-tolerated by patients when proper topical anesthetic is applied beforehand, and it prevents the clinician from experiencing hand fatigue during the injection. The 27-gauge represents the most versatile middle ground, offering a compromise between patient comfort and clinical control, making it the default choice for many everyday dental procedures.
Length Variations and Injection Techniques
In addition to gauges, dental needles are manufactured in different lengths to accommodate the vast anatomical variations found in the human oral cavity. The two standard lengths are typically referred to as "short" and "long." Short needles are generally utilized for localized infiltration anesthesia, where the target area is superficial, such as numbing the upper front teeth for a filling. Long needles are essential for block anesthesia, where the needle must traverse a significant depth of tissue to reach a distant nerve trunk, such as targeting the mandibular nerve near the ramus of the mandible.
Matching Length to the Anatomical Target
Using the incorrect needle length can lead to clinical failure or patient injury. If a short needle is used for a deep block injection, the anesthetic will be deposited in the muscle mass rather than near the nerve, resulting in inadequate numbness. If a long needle is used for a shallow infiltration, the excess length increases the risk of the needle bending, or worse, the tip advancing too deeply and causing trauma to deeper structures. Dentists are trained to assess the patient's facial dimensions—such as the distance from the corner of the mouth to the target nerve—and select the needle length that allows for safe, predictable deposition of the anesthetic agent with minimal excess.
Minimizing Patient Discomfort During Injection
The fear of pain associated with the dental needle is one of the most prevalent causes of dental anxiety worldwide. However, modern dental science has identified that the pain of an injection is rarely caused by the needle puncture itself. Instead, the vast majority of injection pain is caused by the rapid expansion of tissues resulting from the anesthetic solution being injected too quickly. Understanding this physiological reality has led to the development of specific protocols designed to render injections virtually painless.
- Topical Anesthetic Application: Before the needle even touches the tissue, a topical anesthetic gel or spray is applied to the dry mucosa. This numbs the surface nerve endings, effectively eliminating the sharp sting of the initial tissue puncture.
- Slow Injection Rate: The dentist must depress the syringe plunger very slowly, allowing the tissue to gradually accommodate the fluid volume without triggering pain receptors that sense sudden stretching.
- Needle Placement and Stabilization: The needle should be inserted with the bevel facing the bone, and the dentist's hand must be firmly supported to prevent sudden movements. A steady hand prevents the needle from lacerating surrounding tissues.
- Tissue Reciprocation: Keeping the needle stationary and slowly withdrawing it as the injection concludes prevents the needle tip from slicing through tissue layers on its way out.
When these techniques are combined with a sharp, high-quality dental needle, the experience is often described by patients as merely a feeling of "pressure" rather than "pain." The tactile sensitivity of the needle tip also allows the dentist to monitor tissue resistance, adjusting their speed dynamically to ensure patient comfort at all times.
Safety Engineering: Preventing Needlestick Injuries
In a clinical setting, the dental needle presents a significant occupational hazard: the needlestick injury. Accidental punctures can occur during the process of recapping the needle, disassembling the syringe, or disposing of the sharp. Because the needle has been inside a patient's mouth, a needlestick injury carries the potential for transmission of bloodborne pathogens. To combat this, the engineering of dental needles has shifted heavily toward passive and active safety mechanisms.
Modern safety dental needles often incorporate a protective sheath or a retractable mechanism. Some designs feature a hinged shield that the dentist can slide over the needle using a one-handed technique immediately after the injection, locking it in place before the syringe is removed from the patient's mouth. Other advanced systems utilize a spring-loaded mechanism that automatically retracts the needle into the syringe hub the moment the plunger is fully depressed, ensuring the sharp tip is permanently contained. The implementation of engineered safety dental needles has drastically reduced the rate of percutaneous injuries in dental practices, protecting both the dental team and the patients from cross-contamination. The universal adoption of these safety-engineered devices represents a monumental leap forward in occupational health within the dental field.
Infection Control and Single-Use Protocols
The dental needle is strictly classified as a single-use, disposable medical device. Under no circumstances should a dental needle be sterilized and reused on another patient, or even on the same patient for a subsequent injection during the same appointment if it has been withdrawn from the tissue. Once the needle penetrates the mucosa, it becomes contaminated with biological debris, saliva, and potentially blood. Even if visually clean, microscopic organisms can remain trapped within the hollow bore of the needle.
Standard autoclave sterilization protocols, which are highly effective for metal dental instruments like mirrors and forceps, are not considered reliable for the internal lumens of hollow-bore needles. There is a documented risk of prion proteins or resilient bacterial biofilms surviving standard sterilization cycles inside the needle shaft. Therefore, regulatory bodies universally mandate that dental needles are manufactured under sterile conditions, packaged individually, and opened immediately before use. After a single use, the needle must be immediately disposed of in a designated, puncture-resistant sharps container, effectively breaking the chain of infection.
Environmental Considerations and Proper Disposal
While patient safety mandates the single-use nature of dental needles, this protocol generates a substantial amount of medical waste. A standard dental needle assembly consists of stainless steel, medical-grade plastics, and sometimes small amounts of rubber. Because these materials are contaminated with biological fluids, they cannot be processed through standard municipal recycling streams. They must be treated as regulated medical waste.
Dental practices are required by law to maintain clearly labeled, puncture-proof sharps containers in areas where injections are administered and where syringes are disassembled. These containers are designed so that hands cannot reach inside, and they are usually brightly colored and marked with biohazard symbols. Once a sharps container reaches a predetermined fill line—usually three-quarters full to prevent accidental punctures during handling—it is sealed by the facility and handed over to a licensed medical waste management company.
- The waste is typically transported to a specialized treatment facility.
- The most common method of destruction is autoclaving at extremely high temperatures, followed by shredding.
- The shredded, sterilized residue is then safely transported to a landfill.
- Some regions utilize incineration, which reduces the waste to ash, though this method is less favored due to air quality concerns.
Although the environmental footprint of single-use dental needles is non-negligible, the catastrophic risk of cross-infection strictly outweighs recycling efforts. The dental industry continues to research biodegradable components for the hubs and more efficient waste processing technologies, but the stainless steel shaft will likely remain a necessary material due to its required mechanical strength and flexibility.
Addressing Patient Anxiety and Needle Phobia
Trypanophobia, or the severe fear of needles, affects a significant portion of the population and is a leading reason why individuals avoid necessary dental care. The psychological impact of seeing a dental needle can trigger panic attacks, elevated heart rates, and vasovagal syncope (fainting). Addressing this anxiety requires a multifaceted approach that combines empathetic communication with advanced clinical techniques.
One highly effective behavioral strategy is the "tell-show-do" method, where the dentist explains the procedure, demonstrates the equipment without using it, and then performs the injection. Hiding the needle from the patient's line of sight is also a simple yet profoundly effective technique; keeping the syringe out of view until the topical anesthetic has taken effect prevents the anticipatory anxiety spike. Furthermore, modern dental practices often employ adjunctive technologies such as localized vibration devices or computer-controlled local anesthetic delivery systems. These systems slowly and precisely control the flow rate of the anesthetic, often independent of the dentist's hand pressure, which has been shown to significantly reduce the patient's perception of pain and anxiety associated with the dental needle.
For patients with severe phobias, conscious sedation techniques, such as nitrous oxide-oxygen inhalation or oral sedative medications, can be utilized to induce a state of deep relaxation. In these scenarios, the dental needle is still required to achieve local anesthesia, but the patient's heightened state of anxiety is chemically dampened, allowing the clinician to administer the injection safely and efficiently without triggering a stress response.
The Future of Dental Needle Technology
While the fundamental design of the hollow-bore needle has remained relatively consistent for decades, ongoing research aims to further mitigate the drawbacks associated with its use. One area of intense focus is the development of advanced micro-needles. These experimental devices utilize arrays of microscopic needles that are only a fraction of a millimeter in length. Instead of penetrating deep into the muscle to reach a nerve trunk, these micro-needles are designed to deliver anesthetic agents directly into the superficial mucosal layers, where they can diffuse through the tissue to reach the target nerves. Because they are too small to reach pain receptors deep in the tissue, they hold the promise of truly painless injections.
Another frontier is the exploration of needle-free jet injection systems. While early generations of jet injectors were often criticized for being loud, causing bruising, and failing to deliver precise depths of anesthesia, modern engineering has revitalized this concept. Newer jet injection devices use highly compressed springs or precision-controlled pneumatic forces to create a fine, high-pressure stream of anesthetic that penetrates the mucosa. If perfected, these technologies could eventually reduce, though likely not eliminate, the reliance on traditional dental needles for routine procedures. Until such technologies are universally proven safe, reliable, and capable of delivering profound block anesthesia, the traditional dental needle will remain the gold standard in pain management.



 English
English Français
Français русский
русский Español
Español