How to Avoid Common Mistakes When Using an Insulin Syringe?
Apr 08,2026
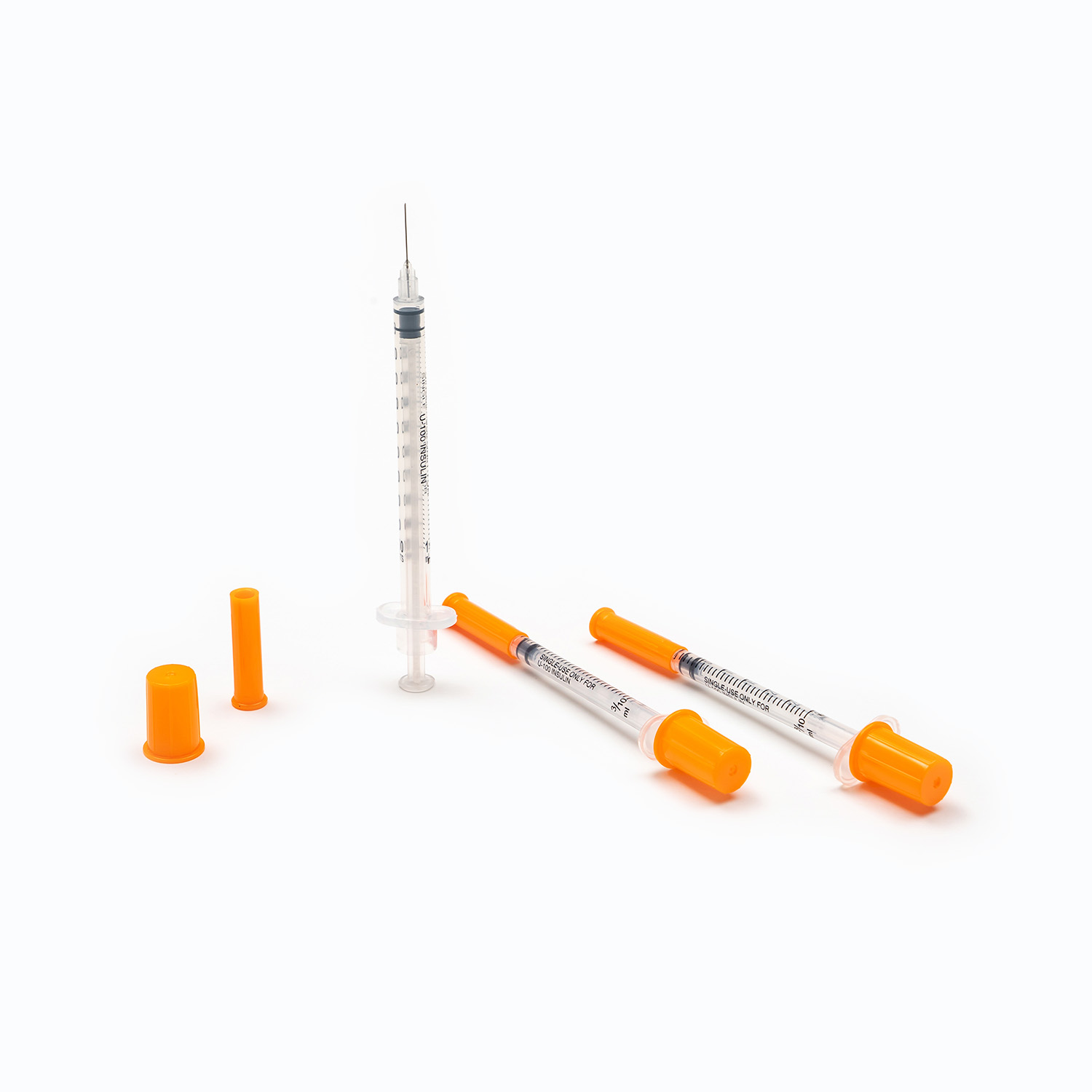
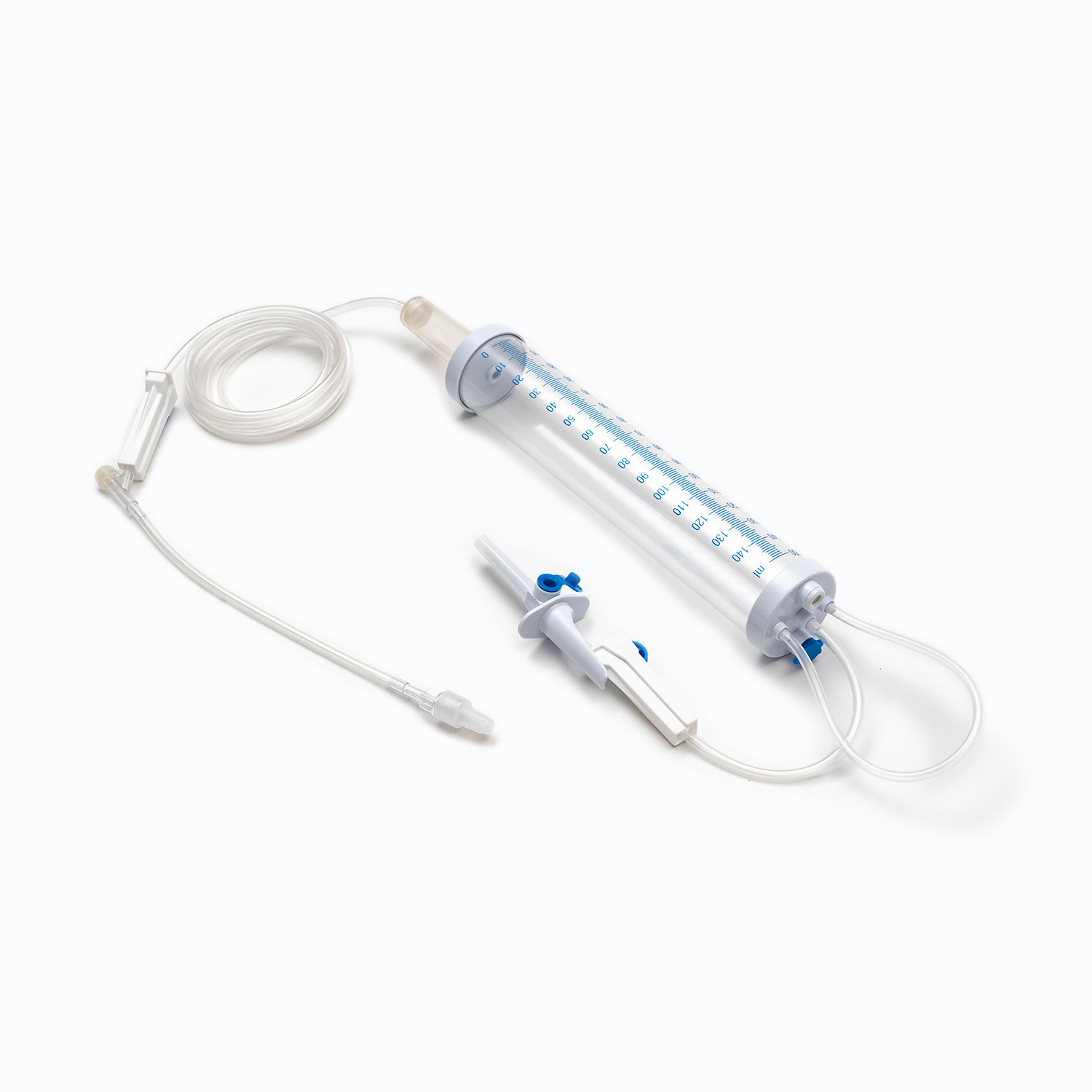
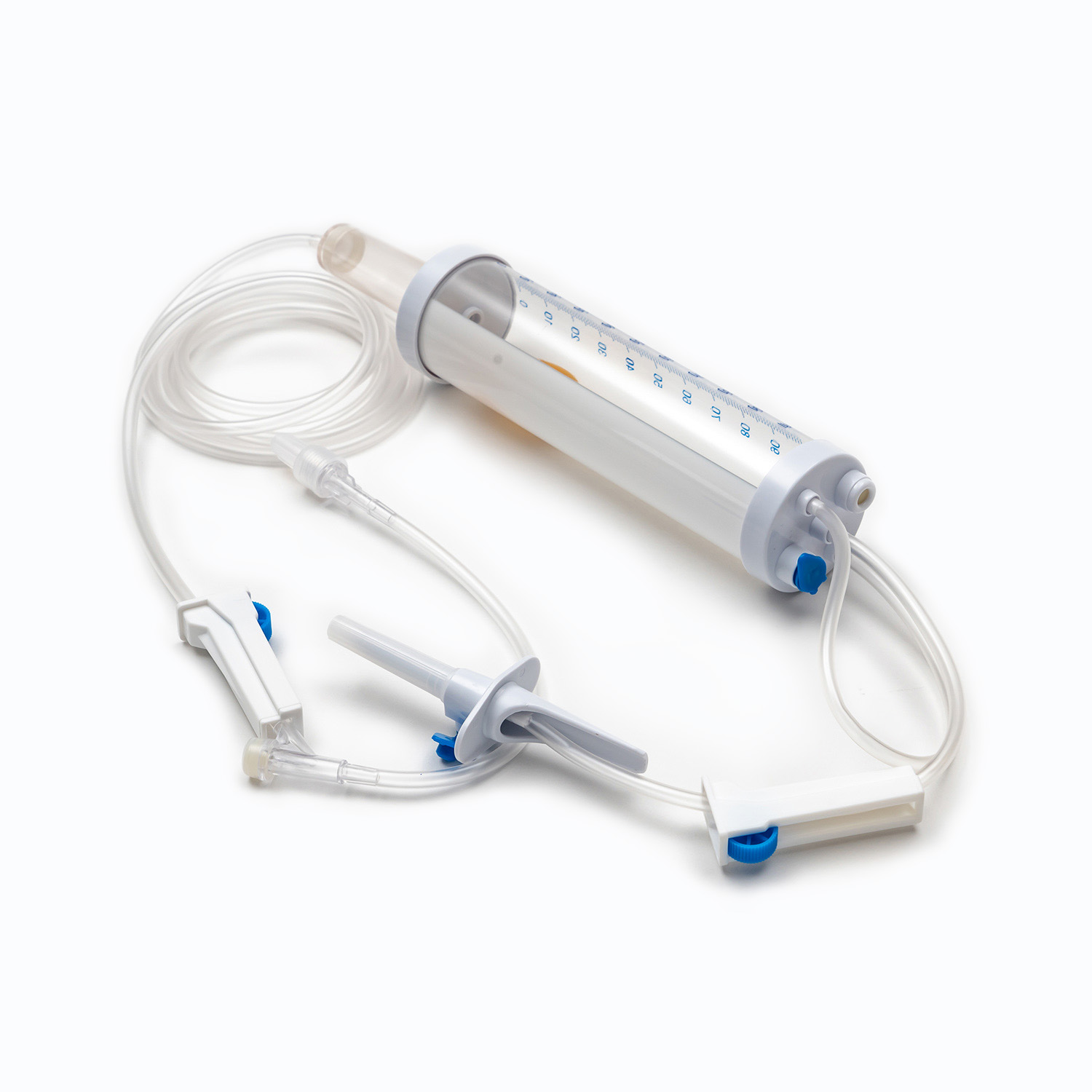
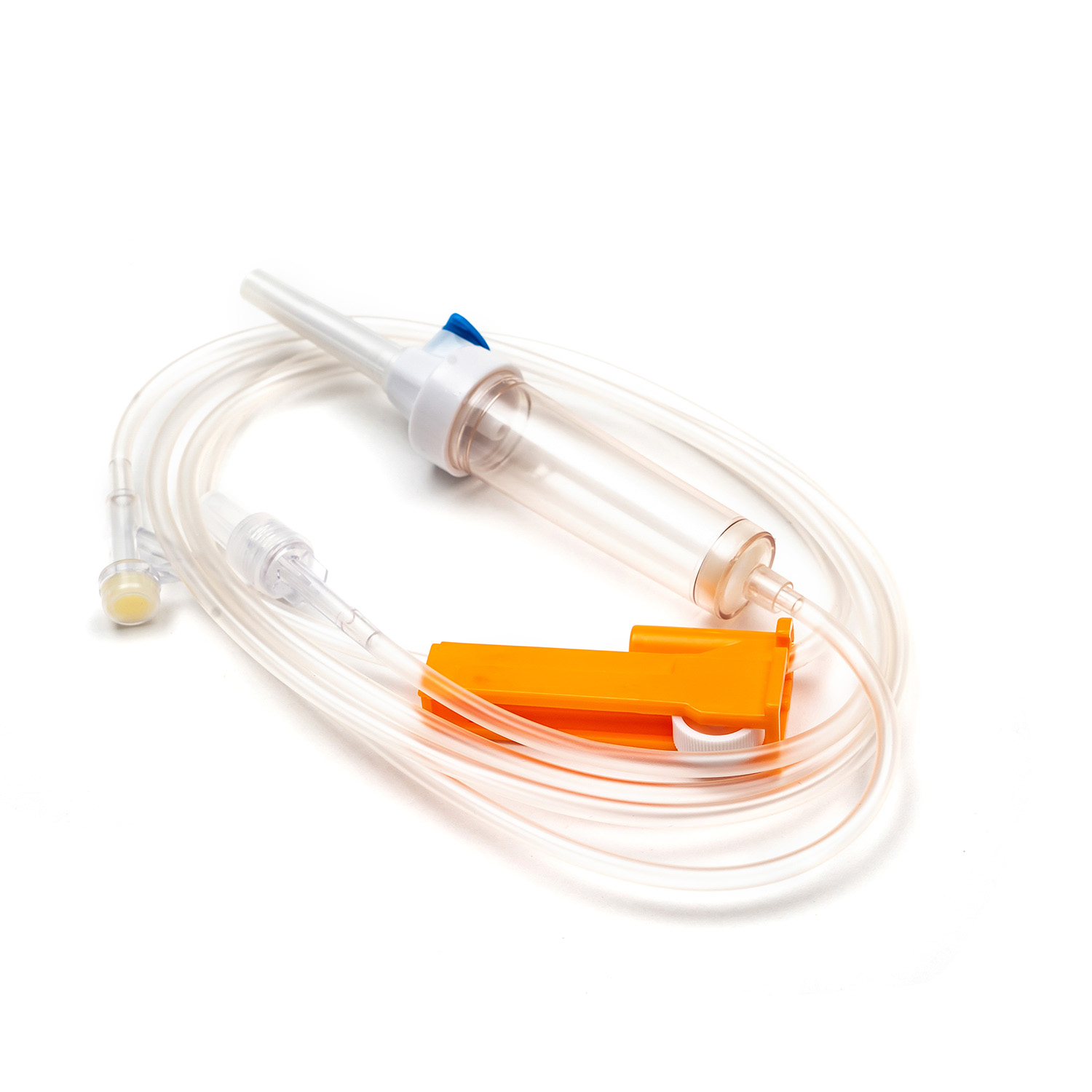
An insulin syringe is a specialized medical device exclusively designed for subcutaneous insulin injection, serving as the most widely used tool for daily insulin delivery among diabetic patients. The core functions of an insulin syringe include accurate insulin measurement, safe penetration into subcutaneous tissue, and precise drug delivery to control blood glucose levels. To ensure therapeutic effects and personal safety, users must select the correct syringe specification, master standard injection techniques, and follow strict disinfection and safety protocols. Single-use insulin syringes are the global mainstream choice, as reusable devices carry high risks of infection, inaccurate dosing, and tissue damage.
The correct application of insulin syringes directly determines the stability of blood glucose control and the quality of life of diabetic patients. Improper use may lead to hypoglycemia, hyperglycemia, local skin infections, lipodystrophy, and other complications. Mastering the full knowledge of insulin syringes is a basic and critical skill for all insulin-dependent patients and their caregivers.
Basic Structure and Components of Insulin Syringes
Insulin syringes are precision-engineered with a simple structure, and every component is customized to match the characteristics of insulin. Understanding each part helps users operate the device correctly and avoid operational errors.
Barrel
The barrel is the main cylindrical body of the syringe, made of transparent medical-grade plastic to allow clear observation of insulin volume and clarity. The surface is printed with clear graduation marks, which are the core basis for accurate insulin extraction. Unlike ordinary syringes, insulin syringe graduations are calibrated in units instead of milliliters, matching the standard measurement unit of insulin. This unique design eliminates conversion errors and ensures dosing accuracy.
Plunger
The plunger is a push-pull rod located inside the barrel, with a tight rubber cap at the top to form a sealed environment. When pulled back, it creates negative pressure to draw insulin into the barrel; when pushed forward, it delivers insulin into the body. The end of the plunger is designed with a non-slip structure for easy operation, especially for elderly patients or those with limited hand strength. The rubber cap fits closely with the inner wall of the barrel to prevent insulin leakage and ensure accurate dose control.
Needle
The needle is the key component for subcutaneous penetration, made of ultra-fine stainless steel with a smooth, lubricated coating to reduce pain and tissue damage during injection. Insulin syringe needles are significantly shorter and thinner than those of intramuscular or intravenous syringes, which is a necessary design to avoid injecting insulin into muscle tissue. Most insulin syringes are equipped with a protective needle cap to maintain sterility before use and prevent needle stick injuries after use.
Flange
The flange is the widened edge at the bottom of the barrel, providing a stable support point for fingers during operation. It helps users fix the syringe stably when drawing and injecting insulin, enhancing operational stability and accuracy. This design is particularly important for patients with poor hand coordination, effectively preventing syringe slippage and dosing errors.
Classification and Selection Criteria of Insulin Syringes
Insulin syringes are classified by capacity, needle length, and needle thickness, and the selection should be based on individual insulin dosage, body shape, skin thickness, and injection habits. Choosing the right syringe is the first step to ensure safe and effective insulin injection.
Classification by Capacity
Capacity is the most core classification indicator, directly matching the patient's single insulin dose. The mainstream specifications are designed to cover the needs of most diabetic patients, and the smaller the capacity, the higher the graduation accuracy.
- Low-dose syringes: Suitable for patients with a single insulin dose of less than 30 units, with ultra-fine graduations to ensure accurate extraction of small doses
- Standard-dose syringes: Suitable for patients with a single dose between 30 and 50 units, balancing accuracy and practicality for daily use
- High-dose syringes: Suitable for patients with a single dose exceeding 50 units, meeting the needs of patients with severe insulin resistance
Classification by Needle Specifications
Needle length and thickness are key factors affecting injection pain, tissue penetration depth, and drug delivery effect. Medical guidelines recommend using thinner and shorter needles for most patients to improve comfort and safety.
| Needle Type | Characteristics | Applicable People |
|---|---|---|
| Short & Thin Needle | Low pain, shallow penetration | Children, thin adults, elderly |
| Standard Needle | Balanced depth and comfort | Average-built adults |
| Long Needle | Deep subcutaneous penetration | Obese patients |
Core Selection Principles
The primary principle of selecting an insulin syringe is that the maximum capacity should be slightly higher than the patient's single dose. Using an oversized syringe for small-dose injection will reduce the accuracy of graduation reading, while using an undersized syringe cannot meet the dose demand. In addition, patients with sensitive skin or fear of pain should prioritize ultra-fine needles; obese patients need to choose longer needles to ensure the drug reaches subcutaneous tissue instead of remaining in the fat layer.
Standard Operation Steps for Insulin Syringes
Standardized operation is the guarantee of accurate insulin delivery and blood glucose control. Non-standard operations such as incorrect extraction, air retention, and wrong injection depth will lead to unstable blood glucose and local tissue damage. The complete operation process is divided into five key steps.
Pre-Operation Preparation
Wash hands thoroughly with soap and clean water, then dry them with a clean towel or disposable paper towel to avoid bacterial contamination. Check the validity period and packaging integrity of the insulin syringe; any damaged, expired, or contaminated syringe must be discarded immediately. Prepare the insulin bottle, and gently roll it between palms for several times if the insulin is cloudy, do not shake vigorously to avoid producing bubbles that affect the dose.
Insulin Extraction
Remove the protective cap from the syringe needle, pull the plunger to draw air into the barrel, with the air volume equal to the required insulin dose. Insert the needle into the insulin bottle, push the plunger to inject air into the bottle to balance the internal pressure. Then invert the bottle and syringe, slowly pull the plunger to extract insulin, ensuring the liquid level is slightly higher than the required graduation. Tap the barrel gently to make air bubbles float to the top, and push the plunger slightly to discharge the bubbles and adjust to the exact dose.
Injection Site Disinfection
Select the appropriate injection site, including the abdomen, outer thigh, upper arm, and buttocks. The abdomen is the preferred site for most patients due to fast and stable insulin absorption. Use a medical disinfectant wipe to clean the skin in a circular motion from the inside to the outside, with a disinfection diameter of not less than a standard size. Wait for the disinfectant to dry naturally before injection, do not blow or wipe the area, otherwise it will reduce the disinfection effect.
Subcutaneous Injection
Hold the syringe like a pen, pinch the disinfected skin gently with the other hand to form a fold (for thin patients), and insert the needle vertically or at a slight angle into the subcutaneous tissue. Push the plunger slowly and evenly to deliver all insulin, do not push too fast to avoid local irritation and pain. After the insulin is completely injected, keep the needle in the skin for a period of time to ensure full drug delivery and prevent leakage.
Post-Injection Disposal
Pull the needle out quickly and gently, press the injection site with a clean cotton swab for a few seconds, and do not rub or massage the area to avoid affecting insulin absorption. Put the used syringe into a special sharp container immediately for safe disposal. Never reuse a disposable insulin syringe, and do not throw it into household garbage at will.
Safe Storage and Maintenance of Insulin Syringes
The storage environment of insulin syringes directly affects their sterility, performance, and service life. Improper storage will lead to needle deformation, barrel damage, and bacterial contamination, bringing potential risks to injection safety.
Unused Syringe Storage Requirements
Store unopened insulin syringes in a cool, dry, and ventilated environment, away from direct sunlight, high temperature, humidity, and sharp objects. The ideal storage temperature is room temperature, avoiding freezing or high temperatures above 30 degrees Celsius. Do not store syringes in the bathroom, kitchen, or car, as these places have large temperature and humidity fluctuations. Keep the original packaging intact before use to maintain sterility and prevent dust and bacterial contamination.
Key Points for On-the-Go Storage
For patients who need to carry syringes when going out, use a special medical storage bag with heat insulation function. Avoid putting syringes in pockets close to the body for a long time to prevent body temperature from affecting the performance of the syringe. When traveling by air, carry syringes in carry-on luggage, do not put them in checked luggage, to avoid loss and damage caused by low temperature and pressure changes in the cargo hold.
Discard and Replacement Standards
Disposable insulin syringes are for one-time use only, and repeated use will cause the needle to become blunt and barbed, increasing injection pain, skin damage, and infection risk. Even if used by the same person, the syringe must be replaced immediately after one injection. Regularly check the stock of syringes at home, and replace all syringes that have expired or damaged packaging in time. Do not use syringes that have been opened and placed for more than a specified time to ensure injection safety.
Common Complications and Prevention Measures
Improper use of insulin syringes can lead to a series of local and systemic complications, which not only affect the therapeutic effect but also damage the physical and mental health of patients. Most complications can be completely avoided by standardizing operations and correcting bad habits.
Local Skin Complications
The most common local complications include redness, swelling, pain, induration, infection, and lipodystrophy at the injection site. Lipodystrophy includes fat atrophy and fat hyperplasia, which are mostly caused by long-term injection at the same site and repeated use of syringes. Fat hyperplasia will affect insulin absorption, leading to unstable blood glucose and increased dosage. Prevention measures include rotating injection sites regularly, using new syringes for each injection, and avoiding injection into damaged or abnormal skin areas.
Systemic Complications
Systemic complications are mainly caused by inaccurate insulin dosing, including hypoglycemia and hyperglycemia. Hypoglycemia is a life-threatening complication, usually caused by excessive insulin extraction or incorrect injection depth, leading to rapid drug absorption. Hyperglycemia is caused by insufficient insulin delivery or drug leakage. In addition, improper disinfection may lead to systemic infection in severe cases. Prevention includes double-checking the dose before injection, mastering the correct injection depth, and monitoring blood glucose changes in real time.
Needle Stick Injuries and Safety Protection
Needle stick injuries are common safety risks for patients and caregivers, which may lead to the transmission of bloodborne pathogens. The core preventive measure is to never recap the needle by hand after use, and to directly put the used syringe into a sealed, sharp container. Replace the sharp container in time when it is full, and do not overfill it. For families with children or pets, store syringes and sharp containers in a locked cabinet to avoid accidental contact and injury.
Best Practices for Optimizing Insulin Syringe Use
On the basis of mastering standard operations, adopting optimized use strategies can further improve the accuracy of insulin delivery, reduce discomfort, and enhance the stability of blood glucose control. These practices are suitable for all insulin-dependent patients and are verified by clinical medical practice.
Injection Site Rotation Management
Establish a regular injection site rotation plan to avoid repeated injection at the same point within a short period. Divide the injection area into multiple small regions, and rotate the injection in sequence, with a distance of not less than a fixed size between adjacent injection points. Consistent rotation can effectively prevent fat hyperplasia and local skin induration, ensuring consistent insulin absorption efficiency every time. Record the injection site daily to avoid random injection, especially for patients who need multiple injections a day.
Injection Technique Optimization
Adjust the injection angle and skin folding method according to individual body shape: thin patients and children need to pinch the skin and inject at an angle to avoid penetrating muscle tissue; obese patients can inject vertically without pinching the skin, ensuring the needle reaches the subcutaneous fat layer. The speed of pushing the plunger should be slow and uniform, which can reduce the stimulation of insulin on local tissue and relieve injection pain. After injection, keeping the needle in the skin for a period of time can effectively prevent insulin leakage from the needle hole.
Dose Verification and Error Prevention
Develop the habit of double-checking the insulin dose before injection, especially for elderly patients with poor eyesight or patients with high daily dose variability. Use a syringe with clear graduations, and ask family members for help to verify the dose if necessary. Avoid using syringes with different graduation standards interchangeably, which is the main cause of dose errors. When mixing two types of insulin, strictly follow the order of extracting fast-acting insulin first and then long-acting insulin to avoid drug contamination and dose deviation.
Adaptation for Special Populations
Elderly patients with limited hand function can choose syringes with anti-slip design and larger flanges to improve operational stability; visually impaired patients can use syringes with raised graduations or ask for assistive devices. Children need special ultra-fine and short needles to reduce pain and fear, and injections should be completed under the supervision of parents. Pregnant women with diabetes need to adjust the injection site and needle length according to the pregnancy stage, avoiding injection on the abdomen in the middle and late pregnancy.
Differences Between Insulin Syringes and Other Insulin Delivery Devices
In addition to insulin syringes, common insulin delivery devices include insulin pens and insulin pumps. Understanding the differences between devices helps patients choose the most suitable delivery tool according to their living habits, economic conditions, and physical conditions.
Comparison with Insulin Pens
Insulin pens are pre-filled with insulin cartridges, with integrated needles and a dose adjustment dial, which are more convenient to carry and operate, and more suitable for patients who go out frequently. Insulin syringes are more cost-effective, with a wider range of dose adjustment, and are suitable for patients with large dose variability and limited economic budget. Insulin syringes require independent extraction of insulin, while insulin pens omit the extraction step, reducing the risk of dose errors. The needles of insulin pens are thinner, bringing lower injection pain, but the overall cost is higher than that of syringes.
Comparison with Insulin Pumps
Insulin pumps are wearable devices that deliver insulin continuously through a subcutaneous catheter, simulating the insulin secretion mode of the human body, with the highest accuracy of blood glucose control, suitable for patients with type 1 diabetes and unstable blood glucose. Insulin syringes are portable and flexible, suitable for intermittent injection, and do not require long-term wearing of equipment. Insulin pumps have high purchase and use costs, require professional training, and have a risk of catheter blockage; insulin syringes are easy to operate, low-cost, and have no complex maintenance requirements.
Core Advantages of Insulin Syringes
Insulin syringes remain the most widely used insulin delivery tool worldwide due to their unique advantages: ultra-low cost, easy availability in medical institutions and pharmacies, simple operation without professional training, wide dose adaptation range, and suitability for all types of insulin. For most type 2 diabetic patients, insulin syringes are the first choice for long-term daily insulin delivery, balancing economy, practicality, and safety. With the improvement of manufacturing technology, modern insulin syringes are continuously optimized in terms of needle fineness, graduation clarity, and operational comfort, further enhancing the user experience.



 English
English Français
Français русский
русский Español
Español